La Antigua Guatemala
La Antigua Guatemala

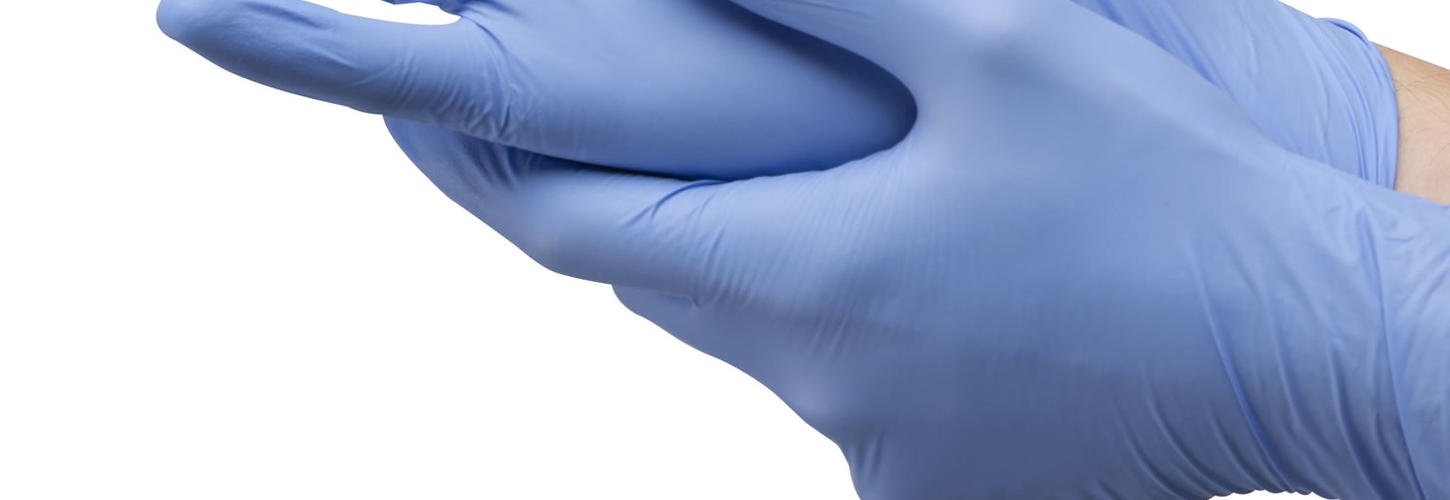
Medical term for a fallen eyelid , mainly the upper eyelid , due to a partial or complete disfunction of the elevador muscle. Causes can be congenital , aquired or degenerative. Can affect one or both eyelids. Aging, constant eyelid trauma due to rubbing in alergies , tumor or cysts heavy enough to cause a fallen eyelid or neurologic are the main causes.
Symptoms of a fallen eyelid that cover the visual axis partially or totally forces the patient to tilt his or her head back to be able to see which causes neck pain and torticollis after some time. Treatment is surgical , the objective of surgery is to repair or strengthen the elevator muscle so the eyelid is lifted to a normal position. Depending each case so is the surgical technique. In children it is important to diagnose and treat in the first years of life , so amblyopia is avoided.
Local anesthesia plus sedation in adults and general anesthesia in children is administered by an anesthesiologist. It is not a painful procedure, scars are very small and slightly visible. the patient can return to his o her normal activities in a short time.
Postoperative period is very short. In children sutures are left in place and they disappear after some time. In adults stitches are removed in a week. Direct exposure to the sun rays must be avoided. Sun glasses must be worn for at least one month , ointment antibiotics and cold compresses are applied.
Complications are infrecuent but if proper care is not given , infection of the surgical wound and its opening can occur. Keloids and hipocorrections can also occur so a second surgery might be needed.
Eliminates excess skin and fat, rejuvenating the appearance of men and women. It is important for the patient to know the results and possible complications of these surgeries to build realistic expectations. Radical changes should not be pursued. Diseases such as Diabetes and High Blood Pressure as well as other systemic diseases should be controlled. These surgeries can be done as a single procedure or combined with others such as eye brow lifting or eyelid ptosis repair ( fallen eyelid).
It is an out patient procedure , local anesthetic and sedation are administered by an anesthesiologist.
We use radiofrecuency technology to perform incisions and skin cuts so less visible scars are obtained. Excess skin and fat are excised. Sutures are left in place for one week. It is not a painful procedure and the patient returns to his /her activities in a short time. It is normal to have swelling and bruising which dissapear in one or two weeks , meanwhile they can be hidden with make up. It is important not to be exposed directly to the sun rays without protection ( sun glasses with UV filters). Visible dark spots and scars may remain if exposed.
Before blepharoplasty is performed a complete ophthalmologic examination to establish a good ocular health, dry eye problems, eyelid malpositions, to recognize the type of skin and take pictures for surgery planning. Previous eye sugeries are not a counterindication for eyelid surgery. Laboratory work up such as coagulation times are required along with other exams : electrocardiogram (EKG) .
The patient must be in good health and should discontinue vitamin suplements , anticoagulant medications such as aspirine and analgesics two weeks before surgery. Even diabetics and High blood pressure patients may have a blepharoplasty , but they should have their diseases well controlled and comply with their medications at all times.
The anatomy and function of the eyelids are better known and understood by an ophthalmologist than any other health professional. Relax in the hands of a specialist , get better results and enjoy of a new and younger expression.
It is a malposition of the eyelids edge turning inwards making the eyelashes touch the cornea and conjunctiva causing irritation , tearing , foreign body sensation , pink eye and infections. Tissue relaxation due to aging, facial nerve paralysis, face and eyelid traumas, scars or previous surgeries can cause it.
In mild cases lubricating drops and gels help the patient. In more severe cases surgery must be performed to bring eyelids edge to a normal position. The technique must be chosen and performed by the EyeMD before corneal scaring appear. Previous to surgery a complete ophthalmologic examination must be performed and pictures taken. It is an outpatient procedure and local anesthesia and sedation is administered by an anesthesiologist. It is not a painful procedure , no eyepatch is placed over the eyelids and the scar is slighly noticeable. The patient can return to his/her normal activities in a short time.
The patient must be in good health before surgery and should discontinue anticoagulants (aspirine), analgesics, vitamin suplements two weeks before surgery. Post operative care includes avoiding direct sun exposure. Apply cold compresses and antibiotic ointment over the surgical wound. Complications are infrecuent ( infections , bad skin scaring) which makes a new surgery necesary.
Lacrimal conduct is the tear excretory system , through it the tears drain to nose and throat. When this conduct is blocked tears don't drain anymore and are spilled to the cheeks, this is called "Epiphora" , which can be very unconfortable and cause cronic eye infections. Causes of lacrimal conduct blockage are nasal alergies , nose traumas , eyelid wounds or have no apparent cause. It is frecuent in the elderly. Diagnosis is made after a complete ophthalmologic examination and special tests are made to determine it in the doctors office.
Dacryocystorhinostomy and silicone tubing is the treatment for lacrimal obstructions. It consists in opening a new pathway to comunicate directly eye and nose. A soft silicone tube is inserted through the punctums ,canaliculi, lacrimal sac and into the nose , and left in place for at least three months.
There are three ways to perform this surgery: 1. External way , through a skin wound . 2. Endonasal or endoscopic (from inside the nose). 3. Laser application .
The most efective way remains to be the external way and is how is done in Centro Visual G&G.
It is an outpatient procedure , general anesthesia is administered by an anesthesiologist. The patient has to rest for a few days to avoid nasal bleeding . Cold compresses and antibiotics in ointment are applied . Stitches are removed one week after surgery.
The patient must be in good health and should discontinue aspirine , anticoagulants and vitamine suplements at least two weeks before surgery. Lacrimal blockage in children is rare and is due to an immaturity in naso-lacrimal conduct formation, which remains closed. Constant pressure and massage throughout the day help open this pathway and no other treatment is needed.
If at age one the child is still tearing ,probing of the lacrimal pathway under sedation is performed. If tearing persists at age five , Dacryocystorhinostomy plus silicone tube is performed.
It is a malposition of the eyelid's edge turning outwards. It is more frecuent in the lower eyelid and it is a common problem of the elderly. Tissue relaxation due to aging, facial nerve paralysis, eyelid trauma, eyelid scars or tumors can cause it. Patients experience tearing , redness , discharge, foreign body sensation, burning because of corneal and conjuntival dryness due to an incomplete closure of the eyelids during sleep.
Mild cases can be treated with lubricating drops and gels, also a patch or a tape placed over the eyelids to keep the eye closed at bed time. More severe cases will need corrective surgery which will bring the eyelids edge to the correct position. Before sugery a complete ophthalmologic examination should be performed and pictures taken. It is an outpatient procedure and local anesthesia is and sedation is administered by an anesthesiologist. The procedure is not painful, no eye patch is necessary and the scar is slighly noticeable.
The patient can return to his/her every day activities in a short time. The patient should be in good health or well controled if his/her diseases . No anticoagulants (aspirine) , analgesics and vitamin suplements should be taken for two weeks before surgery. Post operatory care include avoiding direct sun exposure, antibiotic ointment on the surgical scar and cold compresses. Complications a rare but keloid scar can develop making a second surgery necessary.